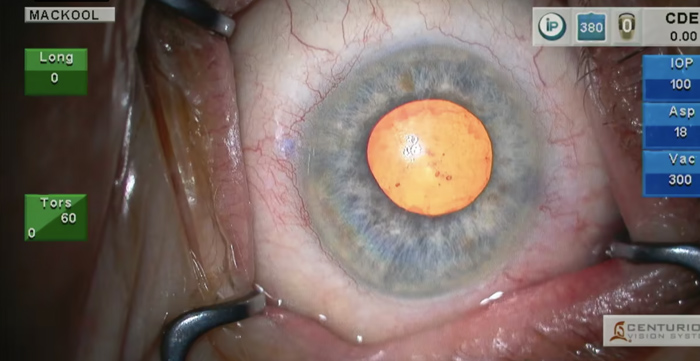
Episode 84: Pseudoexfoliation, Miotic Pupil and Moderate Zonular Laxity
An eye with pseudoexfoliation exhibits moderate zonular laxity and a small pupil that requires enlargement. The options (capsule tension ring, capsule retractors, or a manual
Supported by an unrestricted independent medical educational grant from Alcon
Commercially supported by, Glaukos, MST, and Crestpoint Management
In kind support by Sony Healthcare Solutions

An eye with pseudoexfoliation exhibits moderate zonular laxity and a small pupil that requires enlargement. The options (capsule tension ring, capsule retractors, or a manual
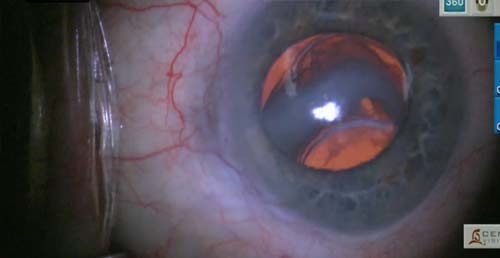
Intravitreal dislocation of a posterior chamber IOL has occurred in the only sighted eye of a 92 year old patient with advanced corneal endothelial cell
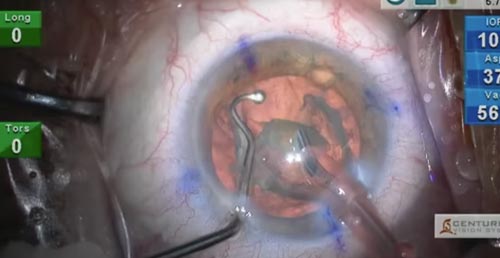
Phacoemulsification of a moderately dense (3+) nuclear cataract is performed. Methods to limit the Cumulative Dissipated Energy (CDE), which indicates the relative amount and magnitude of
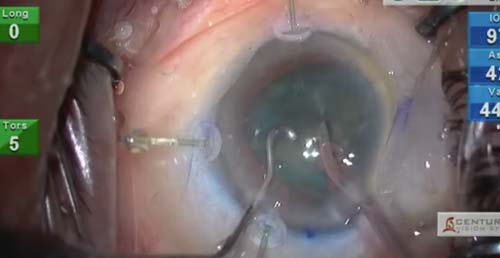
Pseudoexfoliation, zonular laxity, poor dilation, a shallow anterior chamber and a convex anterior capsule are all present in this 85 year old patient.
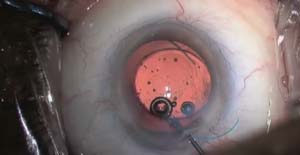
The patient had cataract-implant surgery in her non-dominant eye 6 months earlier, and developed severe dysphotopsia. The decision has been made to proceed with cataract-implant surgery
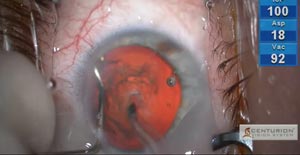
During the early stages of nucleus removal, a large amount of BSS accumulates beneath the conjunctiva and begins to interfere with visualization of the procedure.
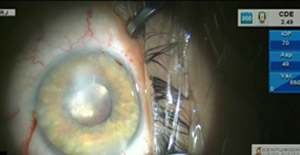
A patient with congenital aniridia undergoes phacoemulsification, IOL insertion, and insertion of an artificial iris device.
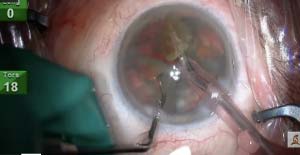
An extremely frail, elderly patient undergoes phacoemulsification performed on her only sighted eye.
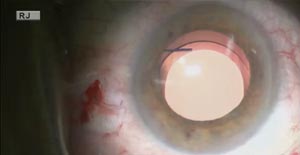
An eye with a decentered and tilted posterior chamber IOL that is fixated to the sclera by the Yamane method undergoes IOL exchange to a
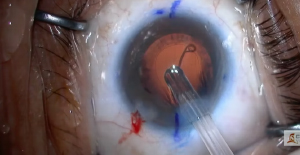
This relatively young patient with clinically obvious pseudoexfoliation and a poorly dilating pupil undergoes phacoemulsification after pupil enlargement and anterior capsule staining.
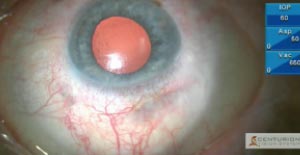
A patient with Marfans syndrome and late posterior dislocation of a sutured single piece PMMA IOL is presented. Methods to reposition and resuture the IOL
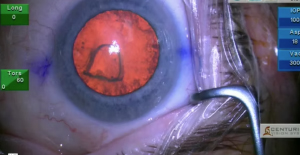
A visible opening in the posterior capsule is present in a post-vitrectomy eye undergoing cataract-implant surgery. Techniques that minimize posterior dislocation of lens material and
Alcon
Glaukos
MST
Crestpoint Management
Amedco

Sony Healthcare Solutions

©2022 Mackool Online CME
Disclaimer: The surgical settings shown in these videos are those of Richard Mackool, MD and RJ Mackool, MD. Viewers should choose settings appropriate to their skill level and the particular case requirements.
Video editing by: J R Snowdon, Inc
Website Design & Production by: stateofthedesign.com