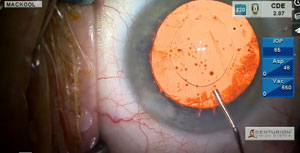
Episode 23: The Aphakic Refraction Technique
Determination of the correct IOL power for a highly myopic eye with posterior staphyloma is fraught with difficulty. Here I employ two methods that can
Supported by an unrestricted independent medical educational grant from Alcon
Commercially supported by, Glaukos, MST, and Crestpoint Management
In kind support by Sony Healthcare Solutions

Determination of the correct IOL power for a highly myopic eye with posterior staphyloma is fraught with difficulty. Here I employ two methods that can
This patient has persistent negative dysphotopsia after cataract-implant surgery performed 18 months ago. A combination of techniques is used to achieve the desired reposition of
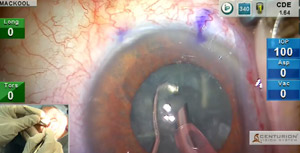
In this case I present a variety of phaco techniques and pearls as cataract extraction and multifocal IOL implantation is performed in an eye with
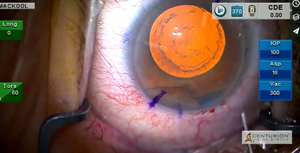
A very interesting case, indeed! Here we will see a patient with considerable head movement, very advanced corneal endothelial dystrophy, pseudoexfoliation, and zonular laxity that
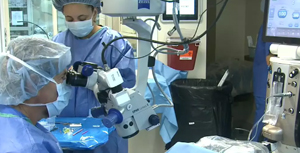
This month’s case features methods for dealing with the problem of a patient with a very active Bell’s Phenomenon. The use and design of my
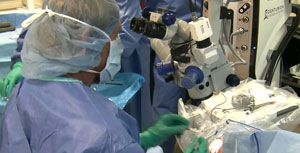
Following a standard cataract procedure, I address the reduction of IOP in this patient with open-angle glaucoma by implanting a stent in the trabecular meshwork.
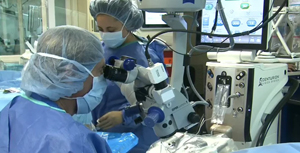
Many patients experience severe photophobia in response to the microscope light. These patients are also often hyperesthetic, and this patient presented with both issues. Here
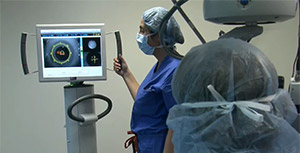
This patient has a dense cataract, low ocular rigidity and unreliable preoperative biometry. The use of a high flow rate of 55 cc/min* to remove
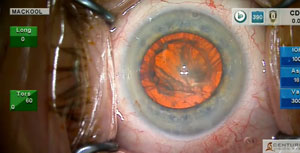
In this issue I discuss and demonstrate the synergism of high IOP and high vacuum settings during phacoemulsification.
Tom is a courageous and engaging young man with advanced Duchenne’s Muscular Dystrophy. Years of steroid treatment have caused him to develop extremely dense cataracts
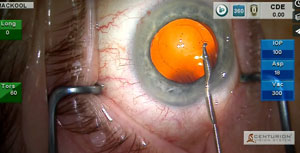
This patient underwent cataract-implant surgery 3 weeks ago, has severe negative dysphotopsia and, fortuitously, a mild hyperopic refractive error.However, the preexisting capsulorhexis is too small
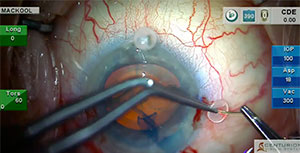
This patient has pseudoexfoliation, shallow anterior chamber, dense nucleus, lax zonule and poor pupillary dilation. I have previously demonstrated the use of capsular retractors for
Alcon
Glaukos
MST
Crestpoint Management
Amedco

Sony Healthcare Solutions

©2022 Mackool Online CME
Disclaimer: The surgical settings shown in these videos are those of Richard Mackool, MD and RJ Mackool, MD. Viewers should choose settings appropriate to their skill level and the particular case requirements.
Video editing by: J R Snowdon, Inc
Website Design & Production by: stateofthedesign.com