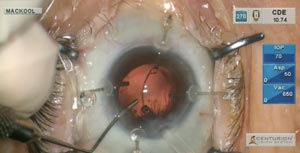
Episode 35: Dense nucleus, lax zonule and capsular tension ring insertion.
Continuing with complicated cases, this month I demonstrate removal of a dense cataract in an eye with zonular laxity and a possible preexisting posterior capsule
Supported by an unrestricted independent medical educational grant from Alcon
Commercially supported by, Glaukos, MST, and Crestpoint Management
In kind support by Sony Healthcare Solutions

Continuing with complicated cases, this month I demonstrate removal of a dense cataract in an eye with zonular laxity and a possible preexisting posterior capsule
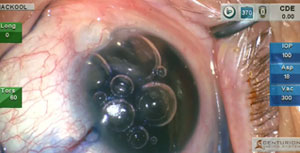
We will finish up our year with 3 rather complex cases. This month, our 57 year old patient is extremely anxious about having cataract surgery.
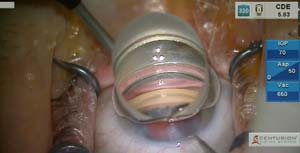
We change it up a bit this month by showing 2 implantations of a stent into the trabecular meshwork in eyes with glaucoma. The first
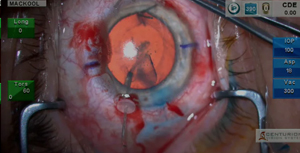
For our viewers who have requested complexity, this one certainly fits the bill: a highly myopic eye with previous retinal detachment, scleral buckle and partial
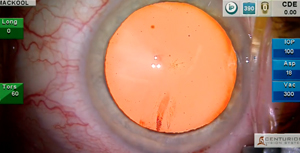
This is a routine case during which I discuss anticipation and prevention of problems caused by patient coughing, infusion misdirection syndrome, and finally the intracameral
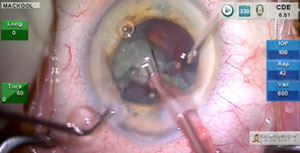
In this case I demonstrate techniques used to remove a dense nucleus in an eye with pseudoexfoliation. Signs of Infusion Misdirection Syndrome and methods to
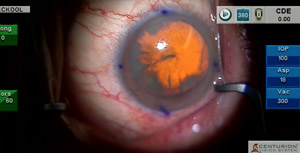
After first removing the anterior subcapsular cataract in a highly myopic patient, I then demonstrate the use of intraoperative aberrometry to confirm the toric IOL
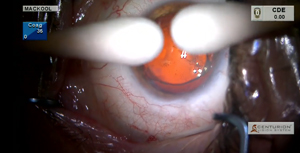
In order to perform cataract surgery upon this non-English speaking patient, I first have to remove an iris-fixated anterior chamber lens implanted 11 years previous.
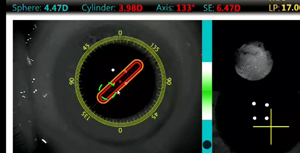
This case demonstrates the use of intraoperative aberrometry plus the Aphakic Refraction Technique to best determine the final IOL power in a keratoconic eye. Tips
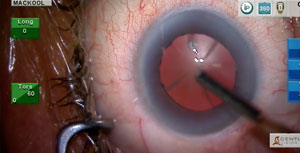
Patience is a critically important trait for all surgeons to develop and maintain. In this patient, Dr Mackool demonstrates its value during removal of a
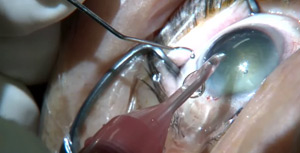
In response to viewer requests, this video demonstrates the Divide and Conquer procedure using a curved ultrasonic needle (Balanced Tip). A useful method of eyelash
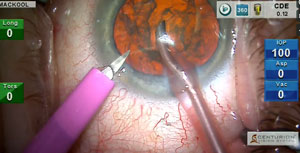
An eye with a shallow anterior chamber is at increased risk for endothelial cell loss during phacoemulsification. A convex anterior capsule increases the risk of
Alcon
Glaukos
MST
Crestpoint Management
Amedco

Sony Healthcare Solutions

©2022 Mackool Online CME
Disclaimer: The surgical settings shown in these videos are those of Richard Mackool, MD and RJ Mackool, MD. Viewers should choose settings appropriate to their skill level and the particular case requirements.
Video editing by: J R Snowdon, Inc
Website Design & Production by: stateofthedesign.com