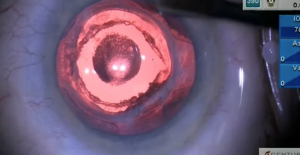
Episode 72: IOL Exchange of a Calcified IOL
After DSAEK, a hydrophilic acrylic IOL develops calcification that requires an IOL exchange
Supported by an unrestricted independent medical educational grant from Alcon
Commercially supported by, Glaukos, MST, and Crestpoint Management
In kind support by Sony Healthcare Solutions

After DSAEK, a hydrophilic acrylic IOL develops calcification that requires an IOL exchange
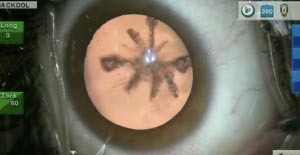
The desired refractive outcome in this patient is the major subject of this video. Consideration of the functional visual field is extremely important, and a
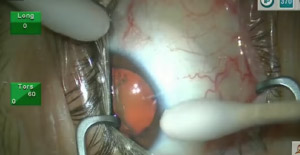
A highly myopic patient requires deep sedation in order to overcome an extremely forceful Bell’s phenomenon. Methods to deal with this problem while maximizing the
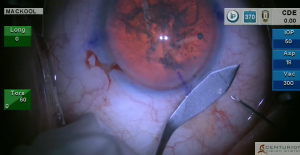
An extremely myopic eye with an increased anterior chamber depth that reduces visibility of the nucleus receives an intravitreal injection to overcome the problem.
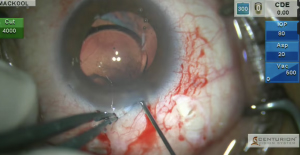
A complex procedure is performed, including pars plana vitrectomy, manual aspiration of residual lens cortex, and elevation and removal of a dislocated IOL from the
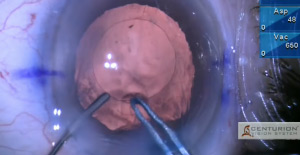
A small posterior capsule opening is converted to a posterior capsulorhexis in an eye with pseudoexfoliation, lax zonule and infusion misdirection syndrome.
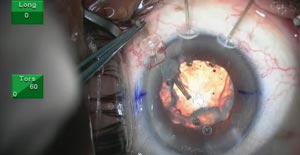
During cataract extraction on an eye with pseudoexfoliation, a poorly dilating pupil, glaucoma and astigmatism, the nasal region of the zonule suddenly fails, enabling vitreous to
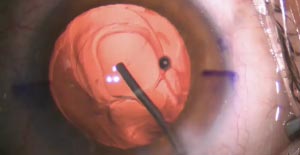
A patient with a potentially problematic degree of corneal coma undergoes cataract–implant surgery with insertion of a diffractive multifocal IOL. Strategies to reduce possible postoperative
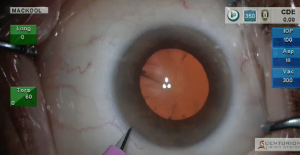
A moderately dense nuclear cataract is removed by phacoemulsification, utilizing techniques that minimize stress on the lens zonule.
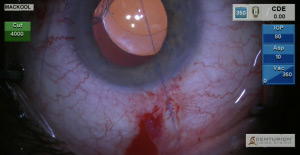
A post-traumatic pupil deformation has caused disabling glare. Two months after complex cataract-IOL surgery with suturing of a capsular tension ring to the sclera and
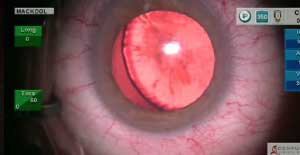
Blunt trauma has caused a subluxated cataract with vitreous prolapse. Phacoemulsification with insertion of 2 capsule tension rings, one of them sutured to the sclera,
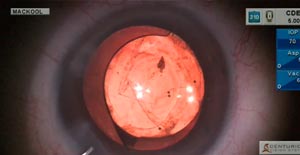
After routine phacoemulsification and IOL insertion, a spontaneous opening in the posterior capsule is observed without obvious cause. A small capsulorhexis must then be enlarged to
Alcon
Glaukos
MST
Crestpoint Management
Amedco

Sony Healthcare Solutions

©2022 Mackool Online CME
Disclaimer: The surgical settings shown in these videos are those of Richard Mackool, MD and RJ Mackool, MD. Viewers should choose settings appropriate to their skill level and the particular case requirements.
Video editing by: J R Snowdon, Inc
Website Design & Production by: stateofthedesign.com